Microbial Therapy Offers New Hope for Vitiligo Patients
A natural compound derived from gut-friendly bacteria significantly slows the progression of vitiligo and may restore pigmentation, reports a new Northwestern University pre-clinical study in mice.
The findings, published in the Journal of Investigative Dermatology, could offer hope to millions affected by the autoimmune disease, which causes visible patches of skin discoloration and carries profound emotional and physical consequences.
“The results in our model were astonishing,” said senior study author I. Caroline Le Poole, a professor of dermatology and microbiology-immunology at Northwestern University Feinberg School of Medicine.
“We found that administering a microbial compound weekly to vitiligo-prone mice significantly suppressed disease progression. It made a spectacular difference in an aggressive model of the disease.”
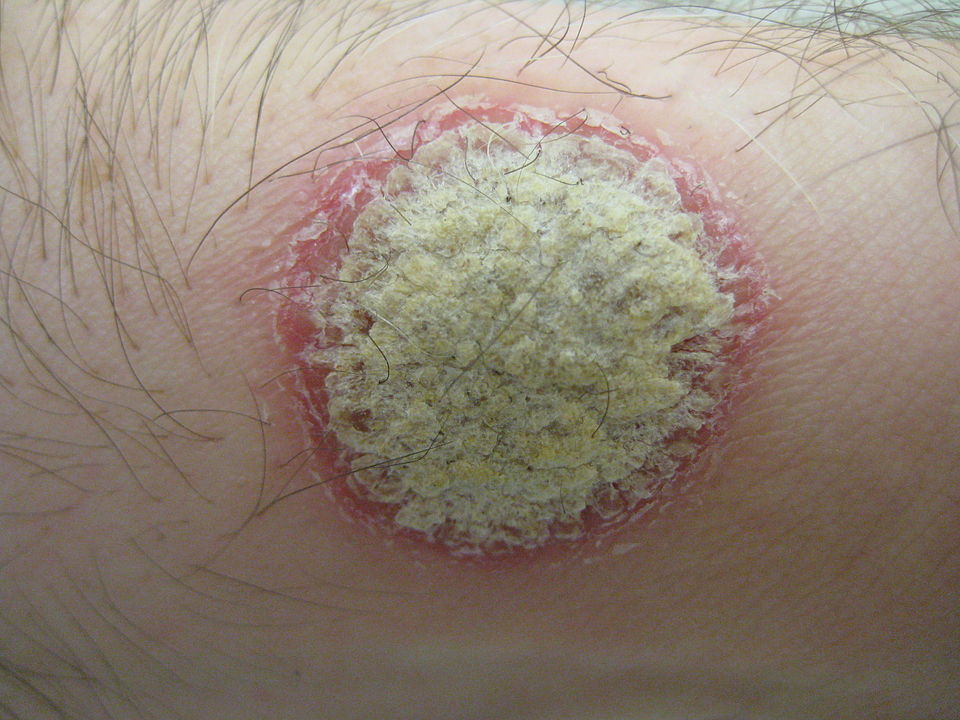
What is vitiligo?
Vitiligo affects 0.5% to 2% of the global population and is linked to other health challenges, including higher risks of cardiovascular disease, psychological distress and endocrine disorders.
Discoloration often appears on the face, scalp, hands and arms, as well as around body openings like the mouth and genitals. Many individuals with vitiligo also have at least one other autoimmune condition.
How the study was conducted
Le Poole and her colleagues administered a microbial product weekly to vitiligo-prone mice over an 18-week period. By the end, pigment loss on the mice’s backs was reduced by 74%.
The product reduced killer T cells that attack the skin’s pigment and increased protective regulatory T cells, which are typically scarce in vitiligo patients.
“This simple microbial compound could work as a standalone therapy, or in synergy with existing treatments,” Le Poole said.
Existing therapy has limitations
In 2022, the FDA approved the first re-pigmentation therapy for vitiligo: Opzelura (ruxolitinib) cream. Clinical trials found that only 30% of patients using the cream regained 75% or more skin re-pigmentation on the face.
“Our findings about the effectiveness of microbial therapy could give hope to patients who are not well-served by existing treatments,” Le Poole said.
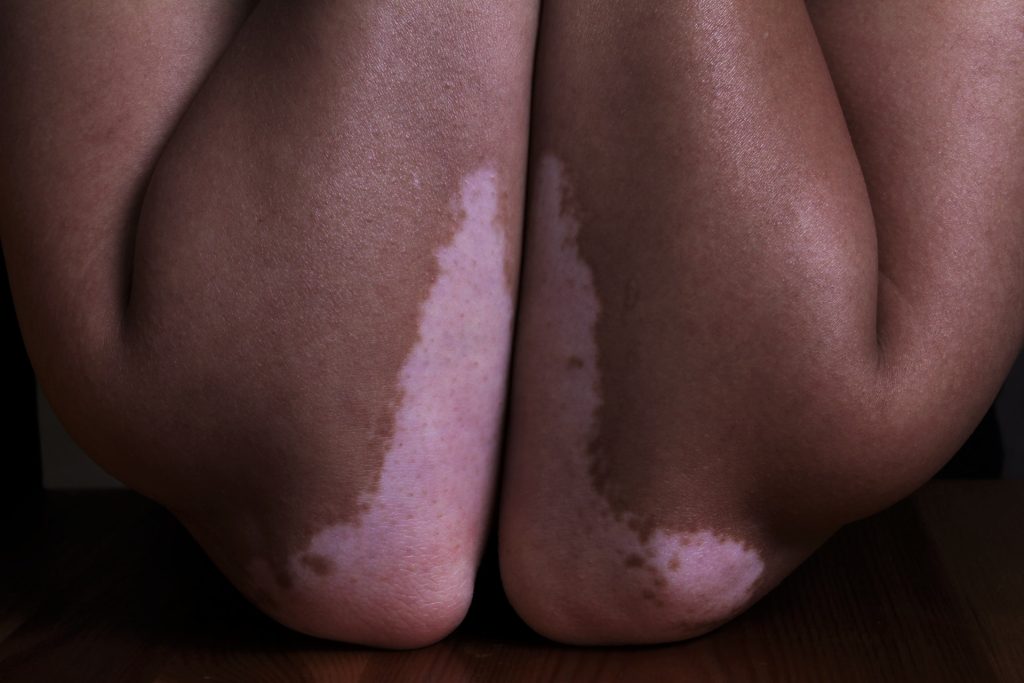
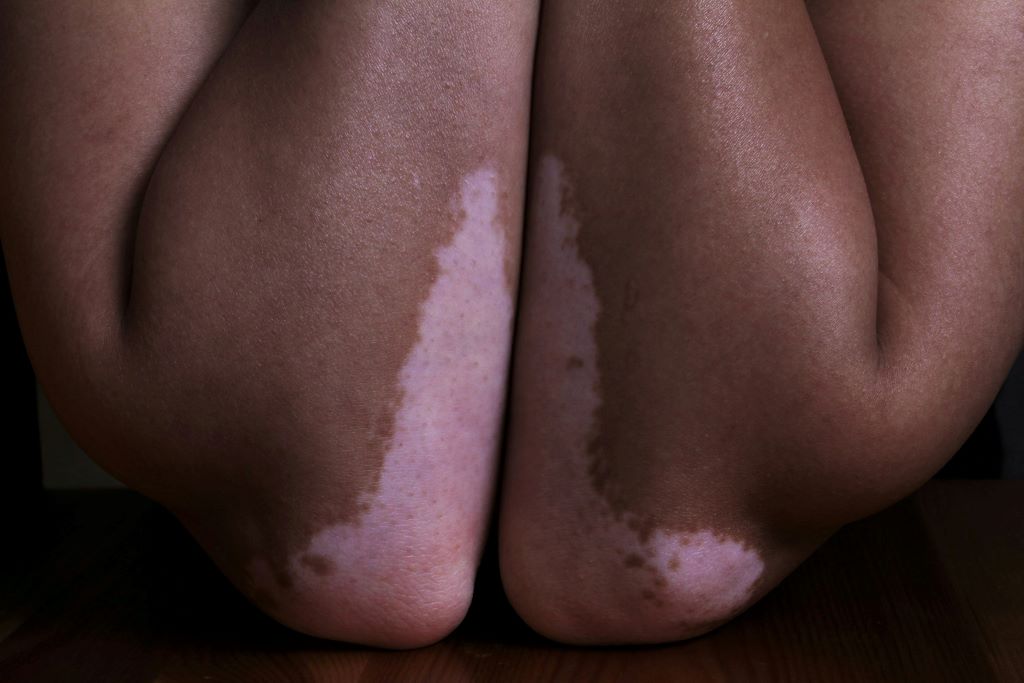
Vitiligo is more severe in patients with darker skin
Le Poole, who has spent more than 30 years studying vitiligo, said the disease has been found to be more severe in people with darker skin tones. The visibility of the discolouration in people with darker skin can also amplify stigma and emotional distress.
“Patients often feel powerless as they watch their disease progress, unsure how they will look next month,” Le Poole said. “For many, stabilising the disease would be life changing.”
While the disease can affect self-esteem – particularly for adolescents navigating social pressures – some people embrace it.
“We’ve seen beautiful models with vitiligo challenging societal norms, and that’s wonderful,” Le Poole added. “But for those who want treatment, it’s important to provide real options that can halt disease progression.”
Next steps
The next challenge is adapting the microbial product for human use. “Weekly injections could work, but we need to explore simpler options, like a food additive or ointment,” said Le Poole. “We also need to understand how long the effects last and the best timing for treatment.”
Le Poole added that the same microbial compound she and her colleagues injected in mice could potentially treat other autoimmune conditions, particularly those involving killer T cells in the skin.
“Our next step is collaborating with scientists from several institutions to refine the compound, understand its mechanisms and determine whether it works alongside existing treatments for auto-immune disease.”
Source: Northwestern University