Case Study: Allmed and Tafta
Empowering Dignified Elder Care Through Compliant, Compassionate Staffing Solutions

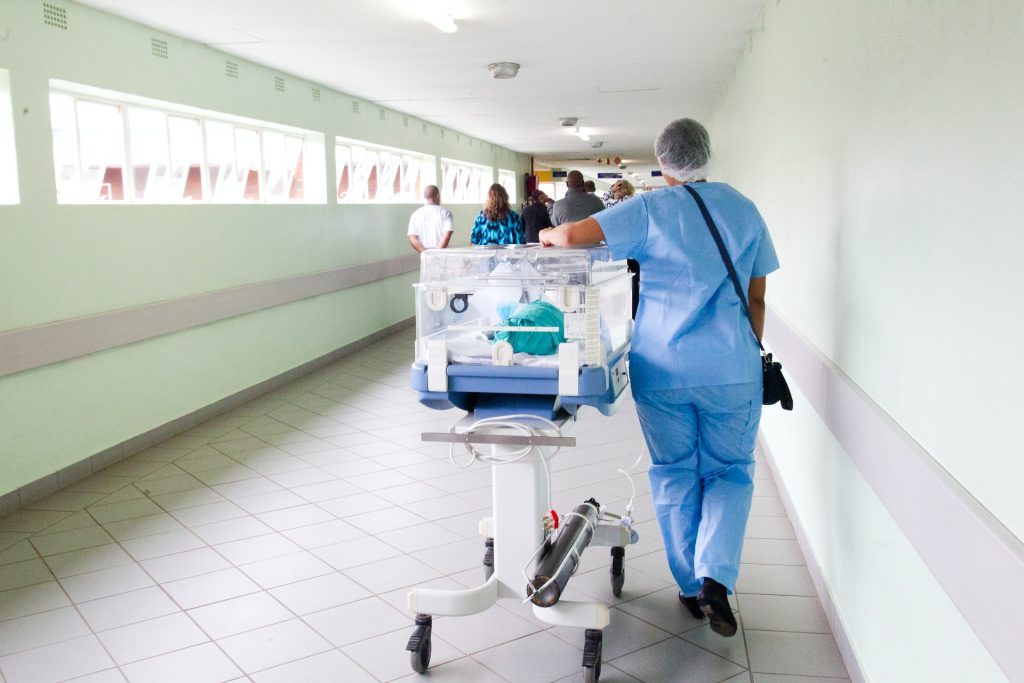
For nearly seven decades, The Association for The Aged (Tafta) has been a cornerstone of care for senior persons in Durban and surrounding communities. Its services include assisted living, frail care, home-based care, meal delivery, and essential social work and advocacy programmes, all designed to support the dignity and well-being of older persons.
Delivering this level of care consistently requires the right professional healthcare staff and strong administrative support across Tafta’s multiple facilities.
The challenge: ensuring compliance and consistency
Recruiting and managing trained Caregivers across several care units can be complex, particularly when strict compliance and accreditation standards must be met. Tafta needed a partner who could supply qualified staff while supporting operational efficiency and upholding care standards. Allmed, a specialist medical personnel solutions provider, with proven experience in healthcare staffing and administration, emerged as the ideal solution.
“At the time we were reviewing our contracts, we considered Allmed as one of the service providers to tender,” explains Yoshina Kistensamy, Divisional Manager: Operations of Tafta.
The requirements were clear: the partner needed to ensure all staff were fully compliant and accredited, while also providing responsive after-contract support. Financial flexibility was equally critical, enabling staffing to scale up or down according to operational realities without penalty.
Allmed provides layered support, with trained professionals backed by clinical facilitators, ensuring both quality care and peace of mind for residents’ families. This support is delivered across three key areas:
- Strategic staffing: Ensures every facility has adequate, skilled personnel and optimises workforce allocation to meet varying needs.
- Compliance oversight: Monitors adherence to healthcare standards, reducing risk and ensuring safe, consistent care practices.
- Hands-on engagement: Provides practical support to staff and enhances day-to-day operations.
By combining these three areas, Allmed enables Tafta to operate efficiently while maintaining a strong focus on the quality and dignity of resident care.
The impact: lifting the burden, prioritising care
The partnership has given Tafta the space to focus on its core mission: providing compassionate care. By outsourcing much of its care staff, Tafta has transferred complex HR responsibilities, including training coordination, on-site supervision, and disciplinary processes, directly to Allmed.
Allmed provides layered support, with trained professionals backed by clinical facilitators, ensuring both quality care and peace of mind for residents’ families. This support is delivered across three key areas:
- Strategic staffing: Ensures every facility has adequate, skilled personnel and optimises workforce allocation to meet varying needs.
- Compliance oversight: Monitors adherence to healthcare standards, reducing risk and ensuring safe, consistent care practices.
- Hands-on engagement: Provides practical support to staff and enhances day-to-day operations.
By combining these three areas, Allmed enables Tafta to operate efficiently while maintaining a strong focus on the quality and dignity of resident care.
The impact: lifting the burden, prioritising care
The partnership has given Tafta the space to focus on its core mission: providing compassionate care. By outsourcing much of its care staff, Tafta has transferred complex HR responsibilities, including training coordination, on-site supervision, and disciplinary processes, directly to Allmed.
“For us, the primary benefit lies in ensuring that our care staff remain fully compliant with all required accreditations and registrations, which supports our commitment to delivering quality care through trained professionals,” says Kistensamy. “In addition, Allmed manages the HR processes, supplementary training, and ongoing supervision for this team, allowing us to focus on expanding and strengthening care and support services for our residents and the broader eThekwini community.”
Allmed’s support goes beyond typical service agreements. They work alongside Tafta’s management and care teams. “Whether it’s a quick phone call, a WhatsApp message, or an on-site visit, Allmed is always available,” Kistensamy adds. “Knowing they are just a message away provides enormous peace of mind.”
Forging a partnership that goes above and beyond
Tafta values the partnership for more than staffing consistency. At the organisation’s annual Sports Day for older persons, Allmed has donated essential items, provided an on-site nurse, and actively participated alongside staff and residents. “It’s not just about supplying caregivers – Allmed consistently shows up and supports our programmes,” says Kistensamy.
Allmed also contributes to Tafta’s fundraising and public-relations events, including the International Day of Care and Support, golf days, resident Christmas lunches, and donor gala dinners. Their willingness to engage with staff, residents, and fellow care partners reinforces Tafta’s values and demonstrates that effective healthcare partnerships are built on the seamless alignment of the organisation, its beneficiaries, and its supporters.
Flexible solutions for non-profit needs
Agility has been a cornerstone of the Allmed–Tafta partnership. When budget pressures arose, Allmed offered alternative staffing rates without compromising service quality.
“They understand our sector and our challenges, and they work with us to make sure our residents are always cared for,” says Kistensamy. Three elements define the success of this collaboration:
- Exceptional customer service: proactive support and responsiveness beyond contractual obligations.
- Flexible staffing solutions: ability to scale services up or down based on resident needs and operational realities.
- Qualified, supported staff: ongoing training, supervision, and guidance ensure consistent, high-quality care.
Through this partnership, Tafta can prioritise its core mission: ensuring every resident receives compassionate, dignified care. With Allmed providing expert staffing and compliance support, the organisation can operate smoothly while maintaining high-quality care standards.