Rooibos Extracts Demonstrate Protective Effects in Preliminary Breast Cancer Research

Rooibos, South Africa’s beloved herbal tisane, with proven benefits for the heart, diabetes management and brain health, is now revealing even more potential in preliminary breast cancer research led by Dr Nicky Verhoog, senior lecturer of biochemistry at Stellenbosch University.

Caption: Dr Nicky Verhoog, senior lecturer of biochemistry at Stellenbosch University.
Oestrogen’s role in breast cancer
While the research is still in its early stages, initial findings suggest that Rooibos extracts may counteract the activity of oestrogen in breast cancer cells – a discovery that has prompted the South African Rooibos Council (SARC) and the Department of Science, Technology and Innovation (DSTI) Sector Innovation Fund Programme to continue to support the work of Dr Verhoog with further studies in animal models scheduled to begin next year.
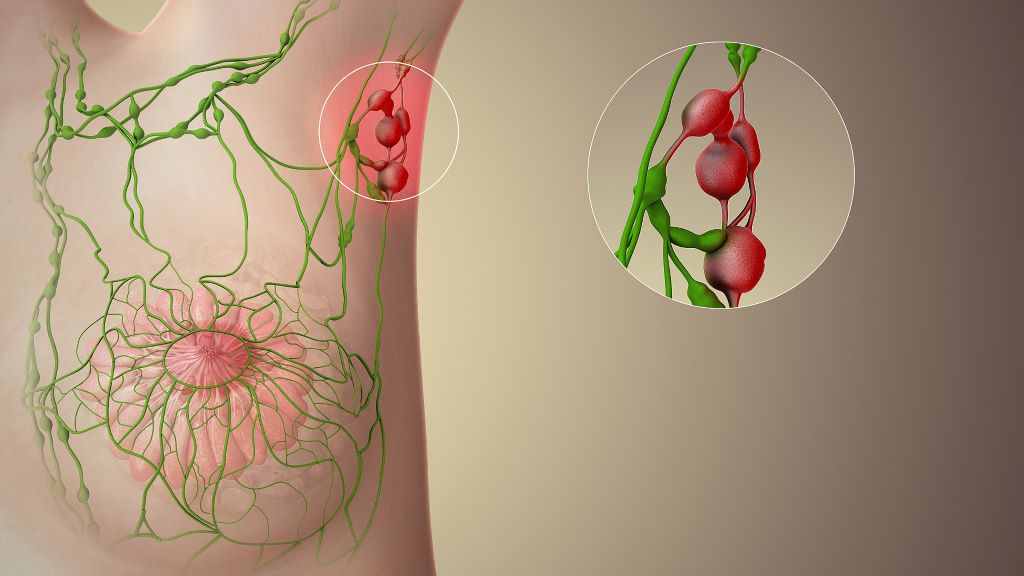
Oestrogen is often described as a kind of driver of breast cancer growth, because many breast cancer tumours carry receptors that respond to it. Although oestrogen doesn’t always start the cancer, it can speed up its growth once the disease has developed. Some newer studies also show that it may sometimes play a more direct role in triggering changes in cells that lead to cancer. Because so many breast cancers are sensitive to oestrogen, the possibility that Rooibos might help block its effect makes these findings especially significant.
Breast cancer in South Africa
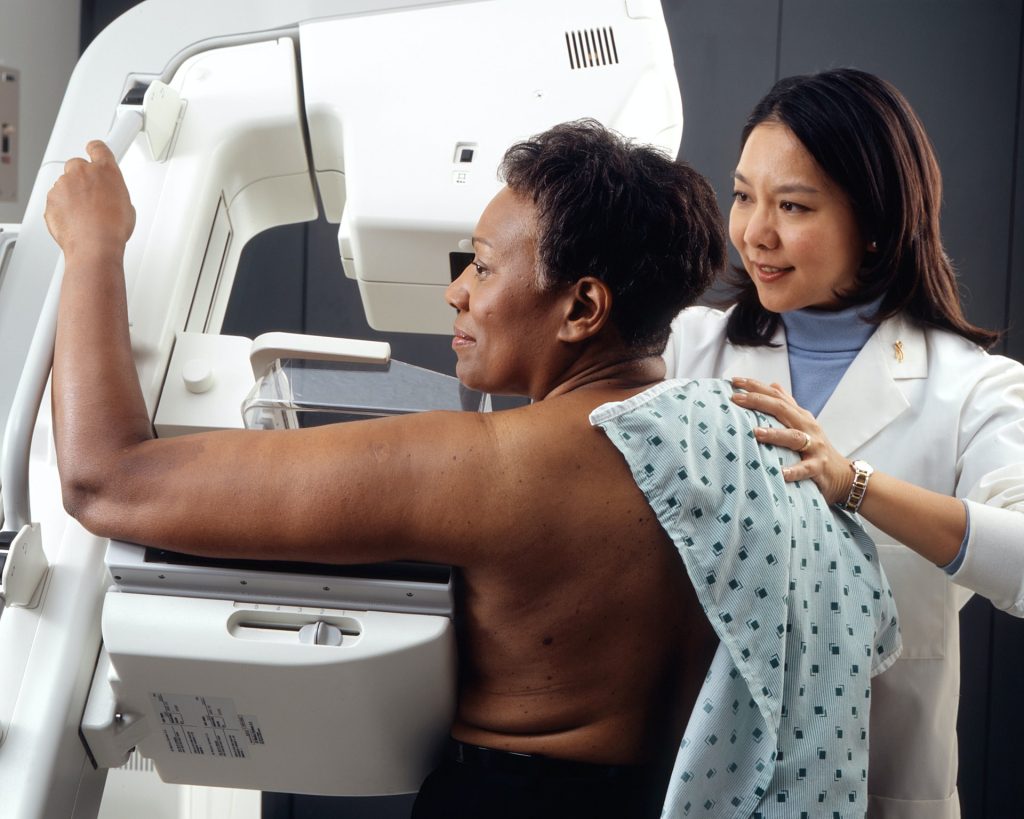
Breast cancer remains a major health concern in the country. According to the latest statistics, between 11 000[1] and 15 000[2] women are diagnosed with breast cancer annually and the disease accounts for approximately 24% of all cancer cases in South African women. Early detection is critical – when identified at an early stage, breast cancer survival rates can exceed 90%, highlighting the importance of regular screening and self-examination.
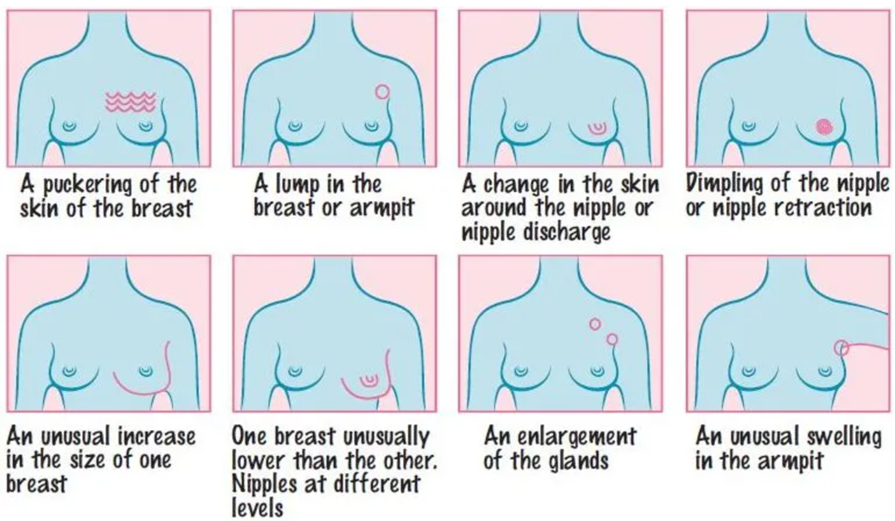
Caption: Warning signs of breast cancer. Source: CANSA (cansa.org.za)
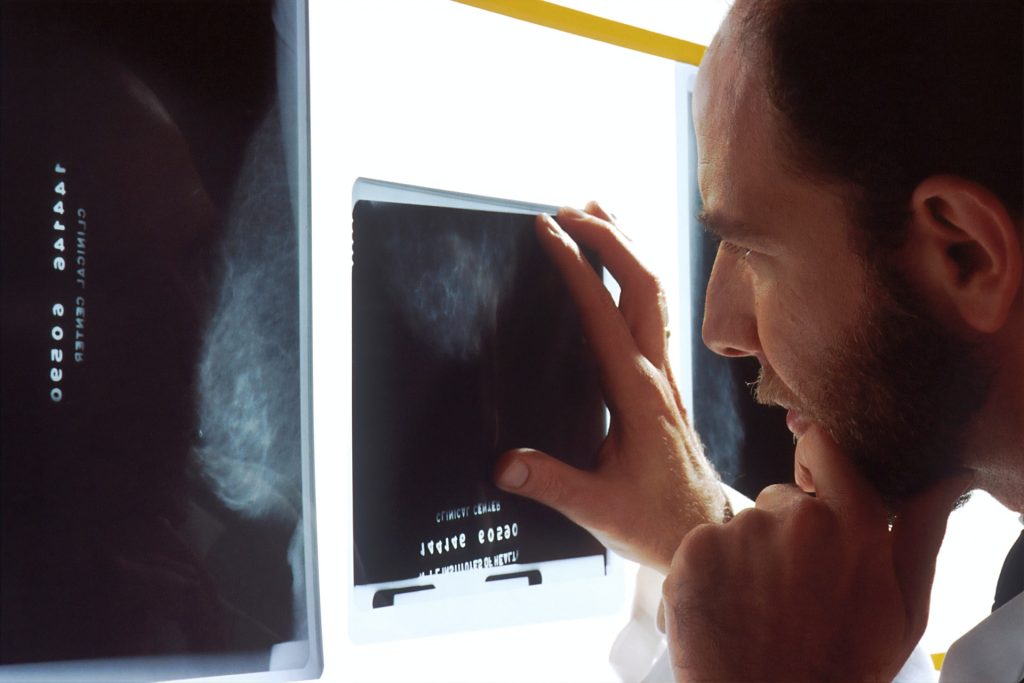
Rooibos under the microscope
Against this backdrop, Dr Verhoog’s team conducted an in vitro (cell) study to examine whether Rooibos could influence oestrogen receptor-positive breast cancer cells. In the past, there has been some uncertainty about whether Rooibos might interact with oestrogen in ways that could affect women with hormone-sensitive breast cancer. This study set out to clarify its role – whether Rooibos could potentially act like estrogen or conversely, help block its activity – and to assess whether it influences cancer cell behaviour.
“To better understand how Rooibos interacts with natural hormones like estrogen, our team wanted to gather clearer scientific evidence,”
Dr Verhoog explains. “We also looked at whether Rooibos could influence the growth and spread of cancer cells, which is especially important for women with hormone-sensitive breast cancer.”
In the laboratory, the researchers worked with well-known breast cancer cell models that carry two types of estrogen receptors: one that can encourage tumour growth (ERα) and another that helps to suppress it (ERβ). They then added Rooibos extracts to see how the cells would respond – in terms of growth, movement and spread.”
The results were encouraging. The extracts acted against oestrogen, in a way similar to fulvestrant, a treatment commonly used to block oestrogen activity in breast cancer treatment. Rooibos slowed down oestrogen-induced cell growth and prevented the cells from spreading. Interestingly, the extracts showed a preference for activating ERβ, the receptor associated with tumour suppression.
“Rooibos appears to act in a protective way against oestrogen-driven breast cancer cells in the lab. It doesn’t mimic oestrogen, but rather inhibits its action. Importantly, we also found that it didn’t interfere with the effect of tamoxifen, a standard breast cancer therapy, which suggests Rooibos could be safely consumed by women undergoing treatment. Of course, this needs confirmation through in vivo (animal) studies.”
Next steps: pre-clinical trials in 2026
While the findings are promising, Dr Verhoog stresses the limitations of in vitro research.
“Lab studies involve single cell types and don’t replicate the complexity of the human body,” she says. “We need to see how Rooibos behaves when metabolised in the body, which is why our next step is pre-clinical trials planned for 2026.”
The next phase of research will move beyond cell studies to look at how Rooibos behaves in a pre-clinical model system. This step is important to confirm its safety for women with oestrogen-sensitive breast cancer and to better understand its effects in the body. The aim is not to test Rooibos as a treatment, but to ensure that it can be safely enjoyed alongside conventional therapies.
Rooibos’s broader health benefits
Rooibos is already celebrated for its wide range of health benefits. Rich in antioxidants and free from caffeine and added sugars, it is a popular alternative to sugary drinks, contributing to overall hydration and general wellness. Previous studies have also highlighted its potential protective effects against other cancer types, including prostate, liver and colon cancers, thanks to its potent antioxidant properties.
“While we are still in the early stages, our research adds to the growing evidence of Rooibos’ multifaceted biological actions. It’s a step toward understanding how this uniquely South African tisane may support health in a variety of ways,” emphasises Dr Verhoog.
Experts stress that these findings should not be interpreted as evidence that Rooibos can prevent or treat breast cancer. Rather, they reinforce its safety for consumption and provide a foundation for future research.
With October recognised as Breast Cancer Awareness Month, the study also underscores the urgent need for continued scientific investigation into the disease, while reminding women that regular screening, awareness of family history and early detection remain the most effective strategies for reducing breast cancer risk and improving outcomes.
[1] https://www.nicd.ac.za/wp-content/uploads/2025/04/NCR_ASR_tables_2023.pdf According to the National Cancer Registry (NCR), 10 980 cases of breast cancer were recorded in 2023. However, CANSA has highlighted significant underreporting, particularly in rural and under-serviced communities, suggesting that the actual number of cases is likely much higher. The available figures are based on pathological diagnoses.
[2] https://pmc.ncbi.nlm.nih.gov/articles/PMC10881925/
The statistics provided by the International Agency for Research on Cancer (IACR) differ from those reported by the South African NCR, with the number of new breast cancer cases in 2020 being much higher in the IACR data than in the NCR data (15,491 versus 9259). These differences are due to the different strategies used to tally the statistics. The NCR is a collection of pathology-based cancer surveillance figures based on the curation of cancer diagnosis data from histology, cytology and bone marrow aspirate and trephine samples; these samples have been collected, analysed and then reported on annually [4]. The IACR data are based on the South African NCR and Eastern Cape Province Cancer Registries.