Fewer Complications When Surgeon–Anaesthesiologist Teams Have Previously Collaborated
Research from ICES, Sunnybrook Research Institute and U of T’s Temerty Faculty of Medicine highlights the potential of using team design to improve patient outcomes

The odds of patient complications following high-risk surgeries is lower when the surgeon and anaesthesiologists have prior experience working together, according to a new study by researchers at ICES, Sunnybrook Research Institute and the University of Toronto.
The findings come from an analysis of data from hundreds of thousands of high-risk surgeries in Ontario over a 10-year period, along with information on the surgeon and anesthesiologist for each procedure and how often the pair had worked together in the previous four years.
The study, which was recently published in JAMA Surgery, highlights the potential of using team design to improve patient outcomes.
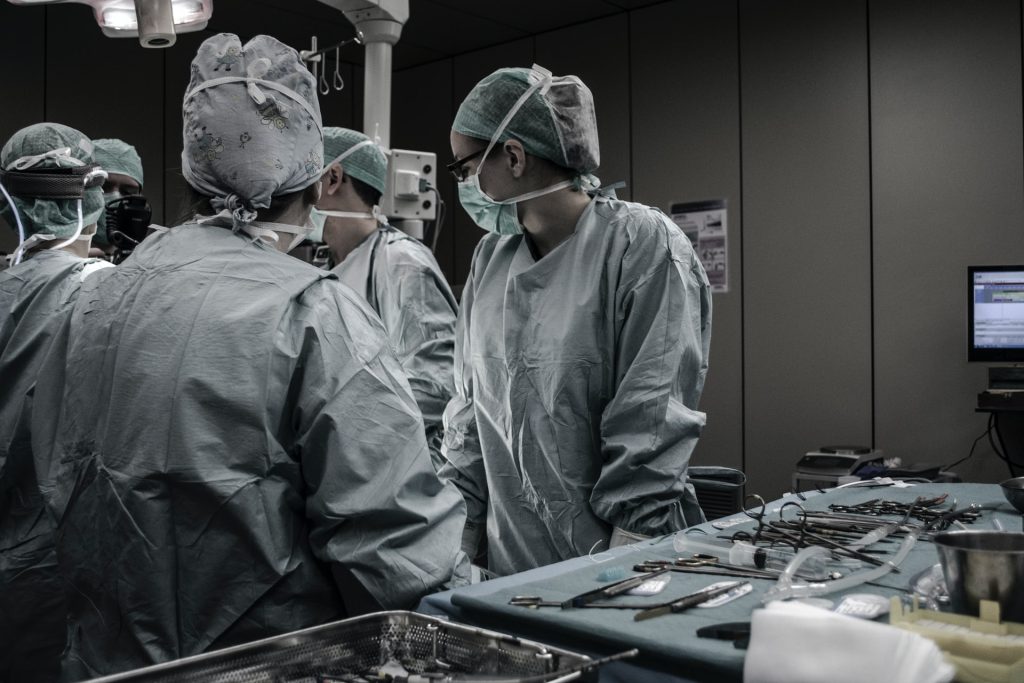
“Team design is used in a lot of other fields like business and sports, but it’s overlooked in health care,” says lead author Julie Hallet, a scientist at Sunnybrook Research Institute and an associate professor of surgery at U of T’s Temerty Faculty of Medicine. “Health care is one of the only areas where we expect people who have never worked together – who sometime have never met before – to perform at peak levels in the most stressful circumstances.”
As a surgeon, Hallet knows first-hand how the environment in an operating room can change depending on team members’ familiarity with each other. It’s something that she and her colleagues have all observed but until recently, lacked the data to describe.
To study this question, Hallet and colleagues analysed population-based health-care data from 711 005 high-risk elective surgeries performed in Ontario between 2009 and 2019, and corresponding information on surgeon-anaesthesiologist teams.
They found that for surgeries related to the gastrointestinal tract, spine and gynaecological cancers, there was an association between surgeon-anaesthesiologist familiarity and the odds of severe complications in the 90 days after surgery – for each additional procedure performed by the same surgeon-anaesthesiologist pair, the likelihood of experiencing a severe complication decreased by three to eight per cent.
“Those are meaningful differences because severe post-operative complications can lead to additional surgeries, ICU stays or even death,” says Hallet.
The researchers also noted that for most procedures, the average surgeon-anaesthesiologist pair were in the operating room together three times a year or less. The exceptions were orthopaedic and cardiac surgery, where surgeons teamed up with the same anaesthesiologist for an average of eight and nine procedures each year, respectively.
These procedures had greater team stability because anaesthesiologists require specialized training to participate in cardiac surgeries and orthopaedic surgeries are often done at dedicated centres like Sunnybrook’s Holland Centre.
“In those particular procedures where they’ve achieved team stability, we do not see an association because the team already has a high degree of familiarity,” says Hallet.
The findings show that unlike expensive new technologies or drugs, optimising the makeup of surgical teams to foster consistency and familiarity could be a no-cost way to improve patient outcomes.
Hallet acknowledges that there are challenges and potential drawbacks to adopting a team design-centred approach to organising and scheduling surgeries. One possible consequence could be that anaesthesiologists, most of whom are currently considered generalists, become increasingly specialised and less comfortable stepping in to cover other procedures.
In the next phase of this project, the researchers are looking at this and other factors that can support the implementation of more stable teams in the operating room.
The team is currently interviewing anaesthesiologists and surgeons to understand their perspectives about the different models of care and what concerns need to be addressed to enable adoption of this new approach. They’re also doing a cost analysis to determine how much money hospitals and health systems could save by having more familiar surgical teams and fewer post-operative complications.
“You can’t put team stability or team familiarity in a bottle or replicate its effects through protocols or processes,” says Hallet.
“The only way that you can get that effect is by putting people together more often and having them work and succeed together.”
Source: University of Toronto