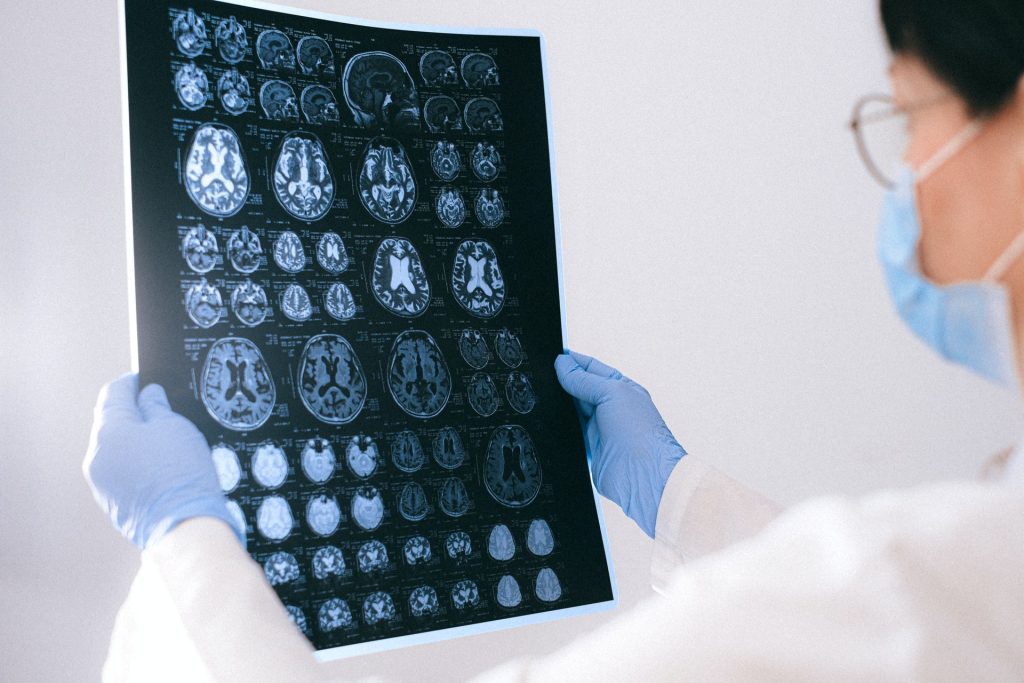
Bone Loss Linked to Cognitive Decline in Women

Researchers have discovered a link between cognitive decline and accelerated bone loss, and found that cognitive decline over five years increased future fracture risk in women. There was a less strong association in men.
The 16-year study enrolling individuals aged 65 and over was led by the Garvan Institute of Medical Research and , and has uncovered a potential new approach to help identify older people who may be at risk of fracture.
“Bone loss and cognitive decline are major public health issues, but both are ‘silent diseases’ that can go undetected and untreated for long periods, often until the conditions are severely progressed,” says Professor Jacqueline Center, Head of the Clinical Studies and Epidemiology lab at Garvan, endocrinologist at St Vincent’s Hospital and senior author of the findings published in the Journal of Bone and Mineral Research.
“Our study has revealed a link between the two in women, which suggests that cognition should be monitored together with bone health, as a decline in one could mean a decline in the other. These findings may help refine best practice guidelines of how cognition and bone health are monitored in older age, to ensure appropriate treatment can be more effectively administered.”
A growing problem with an ageing population
Osteoporosis affects some 200 million people worldwide, and more than 35 million for dementia — numbers set to double over the next 20 years due to rising life expectancy.
“Cognitive decline and bone loss both result in increased disability, loss of independence and an increased risk of mortality. There is some evidence that older individuals with dementia have a higher risk of hip fractures, but whether the decline of both bone and cognitive health are linked over time has not been studied,” said first author Dr Dana Bliuc from the Garvan Institute.
“We set out to understand the long-term association, with our study the first to investigate both cognitive and bone health data over more than 15 years.”
Data was drawn from the Canadian Multicentre Osteoporosis Study (CaMos), which has monitored skeletal health in community-dwelling people since 1995. The researchers examined cognitive and bone health measurements of 1741 women and 620 men aged 65 years and older, who were free of cognitive decline symptoms at the study outset.
Cognition link to bone health
“After adjusting for all other variables, we observed a significant link between a decline in cognitive health and bone loss in women. This association was weaker and not statistically significant in men,” said Dr Bliuc.
“Interestingly, we also saw that cognitive decline over the first five years was associated with a 1.7-fold increase in future fracture risk in women in the subsequent 10 years. This was independent of the level of bone loss,” Dr Bliuc added.
“While this study could not identify a causal link – whether a decline in cognitive function leads to a decline in bone loss, or vice versa – it suggests that cognitive decline should be monitored along with bone health, as a decline in one may signal the need for increased vigilance in the other,” said Professor Center.
The researchers add that the link could potentially be mediated by a third factor, such as oestrogen deficiency, linked to bone loss and cognitive decline. This research also opens the door for additional studies into what the link between these two common conditions may be.
“What our study highlights is that cognitive health is potentially an important factor for providing more information to individuals and their health professionals on fracture risk, and ultimately improve health outcomes for our older population,” said Professor Center.
Source: Garvan Institute of Medical Research
Journal information: Bliuc, D., et al. (2021) Cognitive decline is associated with an accelerated rate of bone loss and increased fracture risk in women: a prospective study from the Canadian Multicentre Osteoporosis Study. Journal of Bone & Mineral Research. doi.org/10.1002/jbmr.4402.