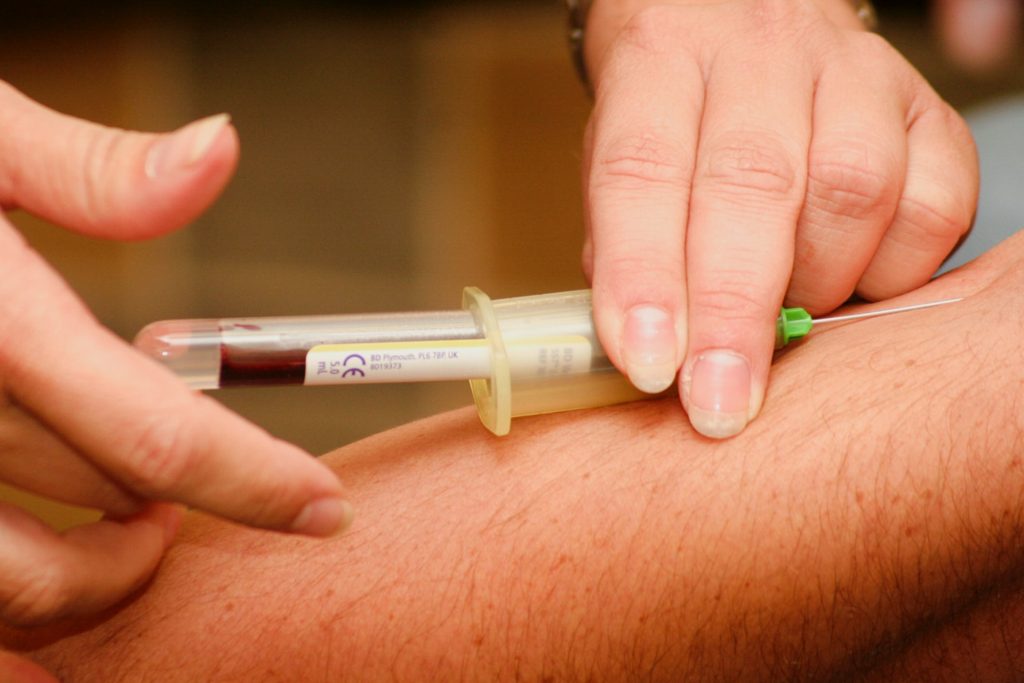
The sleep of hospitalised patients may be often interrupted due to non-urgent blood draws, according to findings from a Yale study published in JAMA. This may be exacerbating sleep deprivation, and putting them at greater risk for health events later on.
In an analysis of more than 5 million non-urgent blood draws collected at Yale New Haven Hospital from 2016 to 2019, a team of researchers found that a high proportion of them occurred during a three-hour window in the early morning.
“We found that nearly four in 10 of total daily blood draws were performed between 4am and 7am,” said César Caraballo-Cordovez, MD, a postdoctoral associate at Yale Center for Outcomes Research and Evaluation (CORE) and co-lead author of the study. “Importantly, we found that this occurred across patients with different sociodemographic characteristics, including older individuals who are at highest risk of adverse health events from sleep deprivation.”
Although early morning blood draws are often considered necessary to inform decisions during morning medical rounds, the authors suggest that sleep interruptions may increase the risk of delirium and other adverse events. “Patients who were recently hospitalised experience a period of generalised risk for myriad adverse health events, a condition named posthospital syndrome,” added Dr Caraballo-Cordovez. “The stress that patients experience during the hospitalisation – including stress from sleep deprivation – is a key contributor to this period of increased risk.”
“This is not an issue at just one hospital,” said Harlan M. Krumholz, MD, SM, professor of medicine and public health at Yale and CORE director. “Our findings reflect an aspect of how inpatient hospital care is being delivered in modern medicine. A more patient-centered care would limit nonurgent tests during sleep hours. However, these early morning blood draws are often considered necessary to make decisions during rounds.”
“We need to re-design our process to protect patients’ sleep, but major changes in our practice must be informed by solid studies that demonstrate the efficacy of strategies to do so without untoward effects,” added Krumholz.
Source: Yale School of Medicine

